Bone
Fractures (Broken Bones)
A fracture is a broken bone. A bone may be completely fractured or partially fractured in any number of ways (crosswise, lengthwise, in multiple pieces).
Types of Fractures
Bones are rigid, but they do bend or “give” somewhat when an outside force is applied. However, if the force is too great, the bones will break, just as a plastic ruler breaks when it is bent too far.
The severity of a fracture usually depends on the force that caused the break. If the bone’s breaking point has been exceeded only slightly, then the bone may crack rather than break all the way through. If the force is extreme, such as in an automobile crash or a gunshot, the bone may shatter.
If the bone breaks in such a way that bone fragments stick out through the skin, or a wound penetrates down to the broken bone, the fracture is called an “open” fracture. This type of fracture is particularly serious because once the skin is broken, infection in both the wound and the bone can occur.
Common types of fractures include:
- Stable fracture. The broken ends of the bone line up and are barely out of place.
- Open, compound fracture. The skin may be pierced by the bone or by a blow that breaks the skin at the time of the fracture. The bone may or may not be visible in the wound.
- Transverse fracture. This type of fracture has a horizontal fracture line.
- Oblique fracture. This type of fracture has an angled pattern.
- Comminuted fracture. In this type of fracture, the bone shatters into three or more pieces.
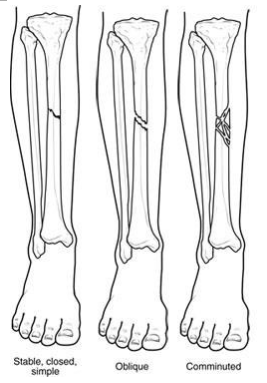
A bone can fracture in different ways. Some common fracture types are shown here.
Cause
The most common causes of fractures are:
- Trauma. A fall, a motor vehicle accident, or a tackle during a football game can all result in fractures.
- Osteoporosis. This disorder weakens bones and makes them more likely to break.
- Overuse. Repetitive motion can tire muscles and place more force on bone. This can result in stress fractures. Stress fractures are more common in athletes.
Symptoms
Many fractures are very painful and may prevent you from moving the injured area. Other common symptoms include:
- Swelling and tenderness around the injury
- Bruising
- Deformity — a limb may look “out of place” or a part of the bone may puncture through the skin
To Top
Doctor Examination
Your doctor will do a careful examination to assess your overall condition, as well as the extent of the injury. He or she will talk with you about how the injury occurred, your symptoms, and medical history.
The most common way to evaluate a fracture is with x-rays, which provide clear images of bone. Your doctor will likely use an x-ray to verify the diagnosis. X-rays can show whether a bone is intact or broken. They can also show the type of fracture and exactly where it is located within the bone.
Treatment
Cast Immobilization
A plaster or fiberglass cast is the most common type of fracture treatment, because most broken bones can heal successfully once they have been repositioned and a cast has been applied to keep the broken ends in proper position while they heal.
Functional Cast or Brace
The cast or brace allows limited or “controlled” movement of nearby joints. This treatment is desirable for some, but not all, fractures.
Traction
Traction is usually used to align a bone or bones by a gentle, steady pulling action.
External Fixation
In this type of operation, metal pins or screws are placed into the broken bone above and below the fracture site. The pins or screws are connected to a metal bar outside the skin. This device is a stabilizing frame that holds the bones in the proper position while they heal.
In cases where the skin and other soft tissues around the fracture are badly damaged, an external fixator may be applied until surgery can be tolerated.
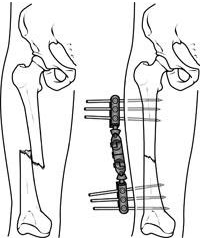
An external fixator applied to a broken femur (thighbone).
Open Reduction and Internal Fixation
During this operation, the bone fragments are first repositioned (reduced) in their normal alignment, and then held together with special screws or by attaching metal plates to the outer surface of the bone. The fragments may also be held together by inserting rods down through the marrow space in the center of the bone.
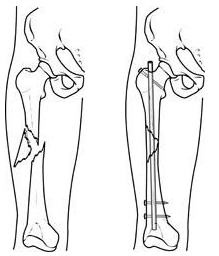
A specially designed metal rod, called an intramedullary nail, provides strong fixation for this thighbone fracture.
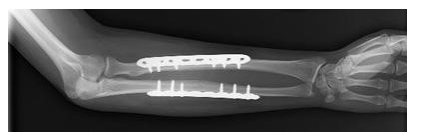
In this x-ray, the broken bones of the forearm are held in position by plates and screws while they heal.
Recovery
Fractures take several weeks to several months to heal, depending on the extent of the injury and how well you follow your doctor’s advice. Pain usually stops long before the fracture is solid enough to handle the stresses of normal activity.
Even after your cast or brace is removed, you may need to continue limiting your movement until the bone is solid enough for normal activity.
During your recovery you will likely lose muscle strength in the injured area. Specific exercises will help you restore normal muscle strength, joint motion, and flexibility.
Prevention
Proper diet and exercise may help in preventing some fractures. A diet rich in calcium and Vitamin D will promote bone strength. Weightbearing exercise also helps keep bones strong.
Osteoporosis
What is osteoporosis?
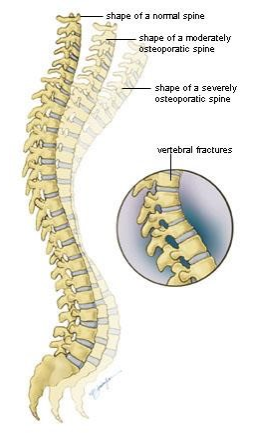
Osteoporosis is a disease of progressive bone loss associated with an increased risk of fractures. The term osteoporosis literally means porous bone. The disease often develops unnoticed over many years, with no symptoms or discomfort until a fracture occurs. Osteoporosis often causes a loss of height and dowager’s hump (a severely rounded upper back).
Why should I be concerned about osteoporosis?
Osteoporosis is a major health problem, affecting more than 44 million Americans and contributing to an estimated 2 million bone fractures per year. According to the National Osteoporosis Foundation, the number of fractures due to osteoporosis may rise to over 3 million by the year 2025.
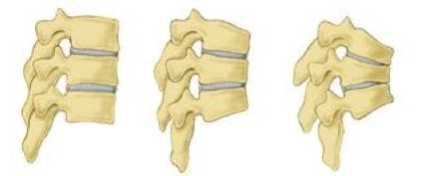
Vertebrae showing signs of osteoporosis. Normal vertebrae (left), vertebrae with mild osteoporosis (center), and vertebrae with severe osteoporosis (right).
One in two women and one in four men older than 50 years will sustain bone fractures caused by osteoporosis. Many of these are painful fractures of the hip, spine, wrist, arm, and leg, which often occur as a result of a fall. However, performing even simple household tasks can result in a fracture of the spine if the bones have been weakened by osteoporosis.
The most serious and debilitating osteoporotic fracture is a hip fracture. Most patients who experience a hip fracture and previously lived independently will require help from their family or home care. All patients who experience a hip fracture will require walking aids for several months, and nearly half will permanently need canes or walkers to move around their house or outdoors. Hip fractures are expensive. Health care costs from hip fractures total more than $11 billion annually, or about $37,000 per patient.
What causes osteoporosis?
Doctors do not know the exact medical causes of osteoporosis, but they have identified many of the major factors that can lead to the disease.
Aging
Everyone loses bone with age. After 35 years of age, the body builds less new bone to replace the loss of old bone. In general, the older you are, the lower your total bone mass and the greater your risk for osteoporosis.
Heredity
A family history of fractures; a small, slender body build; fair skin; and Caucasian or Asian ethnicity can increase the risk for osteoporosis. Heredity also may help explain why some people develop osteoporosis early in life.
Nutrition and Lifestyle
Poor nutrition, including a low calcium diet, low body weight, and a sedentary lifestyle have been linked to osteoporosis, as have smoking and excessive alcohol use.
Medications and Other Illnesses
Osteoporosis has been linked to the use of some medications, including steroids, and to other illnesses, including some thyroid problems.
To Top
What can I do to prevent osteoporosis or keep it from getting worse?
To prevent osteoporosis, slow its progression, and protect yourself from fractures you should include adequate amounts of calcium and Vitamin D in your diet and exercise regularly.
Calcium
During the growing years, your body needs calcium to build strong bones and to create a supply of calcium reserves. Building bone mass when you are young is a good investment for your future. Inadequate calcium during growth can contribute to the development of osteoporosis later in life.
Whatever your age or health status, you need calcium to keep your bones healthy. Calcium continues to be an essential nutrient after growth because the body loses calcium every day. Although calcium cannot prevent gradual bone loss after menopause, it continues to play an essential role in maintaining bone quality. Even if women have gone through menopause or already have osteoporosis, increasing intake of calcium and Vitamin D can decrease the risk of fracture.
How much calcium you need will vary depending on your age and other factors. The National Academy of Sciences makes the following recommendations regarding daily intake of calcium:
- Males and females 9 to 18 years: 1,300 mg per day
- Women and men 19 to 50 years: 1,000 mg per day
- Pregnant or nursing women up to age 18: 1,300 mg per day
- Pregnant or nursing women 19 to 50 years: 1,000 mg per day
- Women and men over 50: 1,200 mg per day
Dairy products, including yogurt and cheese, are excellent sources of calcium. An eight-ounce glass of milk contains about 300 mg of calcium. Other calcium-rich foods include sardines with bones and green leafy vegetables, including broccoli and collard greens.
If your diet does not contain enough calcium, dietary supplements can help. Talk to your doctor before taking a calcium supplement.
Vitamin D
Vitamin D helps your body absorb calcium. The recommendation for Vitamin D is 200-600 IU (international units) daily. Supplemented dairy products are an excellent source of Vitamin D. (A cup of milk contains 100 IU of Vitamin D. A multivitamin contains 400 IU of Vitamin D.) Vitamin supplements can be taken if your diet does not contain enough of this nutrient. Again, consult with your doctor before taking a vitamin supplement. Too much Vitamin D can be toxic.
Exercise Regularly
Like muscles, bones need exercise to stay strong. No matter what your age, exercise can help minimize bone loss while providing many additional health benefits. Doctors believe that a program of moderate, regular exercise (3 to 4 times a week) is effective for the prevention and management of osteoporosis. Weight-bearing exercises such as walking, jogging, hiking, climbing stairs, dancing, treadmill exercises, and weight lifting are probably best. Falls account for 50% of fractures; therefore, even if you have low bone density, you can prevent fractures if you avoid falls. Programs that emphasize balance training, especially tai chi, should be emphasized. Consult with your doctor before beginning any exercise program.
How is osteoporosis diagnosed?
The diagnosis of osteoporosis is usually made by your doctor using a combination of a complete medical history and physical examination, skeletal x-rays, bone densitometry, and specialized laboratory tests. If your doctor diagnoses low bone mass, he or she may want to perform additional tests to rule out the possibility of other diseases that can cause bone loss, including osteomalacia (a metabolic bone disease characterized by abnormal mineralization of bone) or hyperparathyroidism (overactivity of the parathyroid glands).
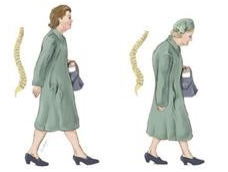
Loss of height and a stooped appearance of a person with osteoporosis results from partial collapse of weakened vertebrae.
Bone densitometry is a safe, painless x-ray technique that compares your bone density to the peak bone density that someone of your same sex and ethnicity should have reached at 20 to 25 years of age.
Bone densitometry is often performed in women at the time of menopause. Several types of bone densitometry are used today to detect bone loss in different areas of the body. Dual-energy x-ray absorptiometry (DEXA) is one of the most accurate methods, but other techniques can also identify osteoporosis, including single photon absorptiometry (SPA), quantitative computed tomography (QCT), radiographic absorptiometry, and ultrasound. Your doctor can determine which method is best suited for you.
To Top
How is osteoporosis treated?
Because lost bone cannot be replaced, treatment for osteoporosis focuses on the prevention of further bone loss. Treatment is often a team effort involving a physician or internist, an orthopaedist, a gynecologist, and an endocrinologist.
Although exercise and nutrition therapy are often key components of a treatment plan for osteoporosis, there are other treatments as well.
Estrogen Replacement Therapy
Estrogen replacement therapy (ERT) is often recommended for women at high risk for osteoporosis to prevent bone loss and reduce fracture risk. A measurement of bone density when menopause begins may help you decide whether ERT is right for you. Hormones also prevent heart disease, improve cognitive functioning, and improve urinary function. ERT is not without some risk, including enhanced risk of breast cancer; the risks and benefits of ERT should be discussed with your doctor.
Selective Estrogen Receptor Modulators
New anti-estrogens known as SERMs (selective estrogen receptor modulators) can increase bone mass, decrease the risk of spine fractures, and lower the risk of breast cancer.
Calcitonin
Calcitonin is another medication used to decrease bone loss. A nasal spray form of this medication increases bone mass, limits spine fractures, and may offer some pain relief.
Bisphosphonates
Bisphosphonates, including alendronate, markedly increase bone mass and prevent both spine and hip fractures.
ERT, SERMs, calcitonin, and bisphosphonates all offer patient with osteoporosis an opportunity to not only increase bone mass, but also to significantly reduce fracture risk. Prevention is preferable to waiting until treatment is necessary.
Your orthopaedist is a medical doctor with extensive training in the diagnosis and nonsurgical and surgical treatment of the musculoskeletal system, including bones, joints, ligaments, tendons, muscles and nerves.
This has been prepared by Prof.Bilal Obeid and is intended to contain current information on the subject from recognized authorities. However, it does not represent official policy of the all orthopedist and its text should not be construed as excluding other acceptable viewpoints.
Your orthopedist is a medical doctor with extensive training in the diagnosis and nonsurgical and surgical treatment of the musculoskeletal system, including bones, joints, ligaments, tendons, muscles and nerves.
This has been prepared by Prof. Bilal Obeid and is intended to contain current information on the subject from recognized authorities. However, it does not represent official policy of the all orthopedist and its text should not be construed as excluding other acceptable viewpoints.

Address 1
Tebnin, infront of tebnin hospital
Address 2
Tyre, next to Al – Mashrek center
Social Media
Contact Us
- +961 70 125528
- info@bilalobeid.com
